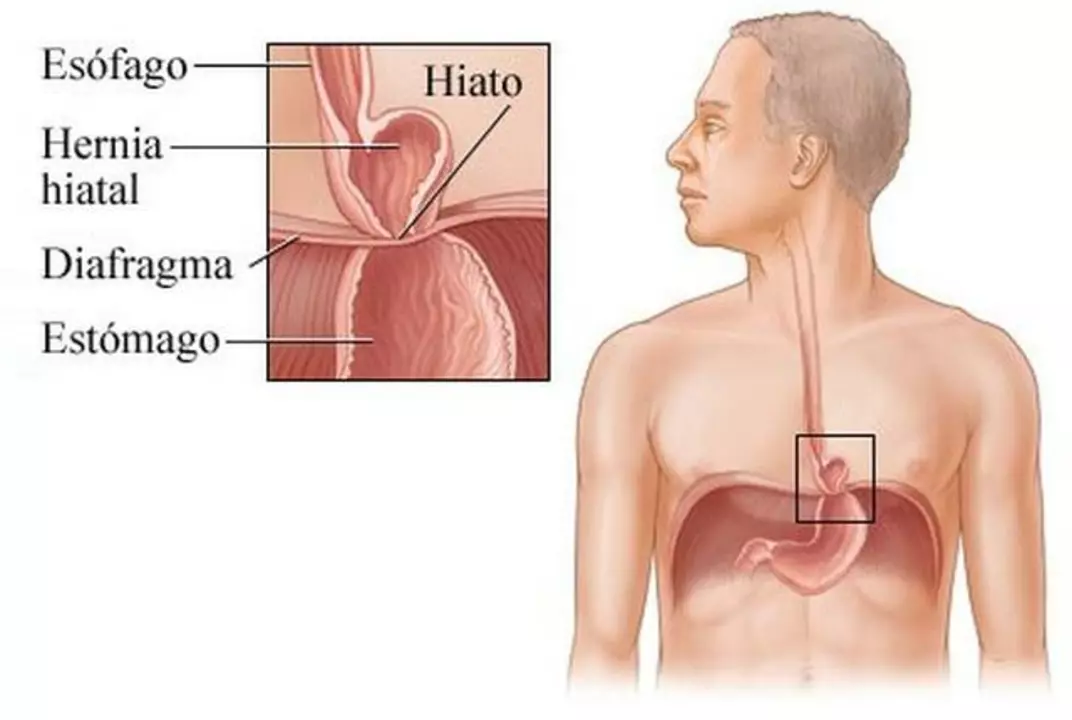
Here’s a clear fact: many people have a hiatal hernia and don’t know it. A hiatal hernia happens when part of your stomach pushes up through the diaphragm into the chest. That can make acid reflux worse, cause chest or upper belly pain, and mess with sleep. You don’t need to panic, but you should know what to watch for and what actually helps.
Symptoms range from mild to annoying: heartburn, regurgitation of food or acid, trouble swallowing, belching, and chest discomfort. If you feel sudden severe chest pain, shortness of breath, fainting, or vomiting that won’t stop, get emergency help — those can mean a serious problem. Otherwise, if reflux or chest pressure happens more than a few times a week, see your doctor for a simple check-up.
Doctors usually suspect a hiatal hernia from your symptoms. They may order tests: an upper GI X-ray, endoscopy (a camera down the throat), or pH monitoring to measure acid in the esophagus. These tests tell whether the hernia is small and harmless or large and causing real trouble.
First line care often starts at home. Try these changes: eat smaller meals, avoid lying down within two to three hours after eating, raise the head of your bed by 6–8 inches, and cut back on alcohol, caffeine, spicy foods, and fatty meals. Smoking also weakens the valve between the stomach and esophagus — quitting helps.
Over-the-counter antacids or H2 blockers can calm symptoms short-term. If reflux keeps coming back, doctors prescribe proton pump inhibitors (PPIs) like omeprazole for a few weeks to months. PPIs reduce acid and give damaged tissue a chance to heal. Always follow dosing guidance and check interactions with other drugs you take.
Surgery is reserved for people who don’t respond to medications or who have a large hernia causing swallowing problems or anemia from bleeding. The common operation is a laparoscopic repair where the stomach is moved back and the opening in the diaphragm is tightened. Many patients do well after surgery, but it’s not risk-free — talk options through with a GI surgeon.
Want quick symptom relief during a flare? Try chewing sugar-free gum after meals to boost saliva and clear acid, and choose lean proteins, cooked vegetables, and whole grains that sit easier in the stomach. Avoid tight belts and heavy lifting that push on your abdomen.
If you’ve been living with reflux for a long time, ask your doctor about screening for Barrett’s esophagus, a change in the esophagus lining linked to long-term acid exposure. Early detection changes how doctors follow you.
Bottom line: small lifestyle changes often cut symptoms a lot. If symptoms are frequent, severe, or sudden, get medical advice. You can manage a hiatal hernia — and sleep, eat, and move with far less discomfort when you take the right steps.
In a recent blog post, I discussed the potential benefits of Ranitidine in providing relief for those suffering from hiatal hernia. As a popular medication for reducing stomach acid production, Ranitidine may help alleviate the symptoms associated with this condition. Many people have found relief through its use, but it's important to note that it may not work for everyone. As always, it's crucial to consult with a medical professional before starting any new treatment. Overall, Ranitidine could be a viable option for those seeking relief from the uncomfortable symptoms of a hiatal hernia.
