Fungal skin discoloration happens when common skin fungi change pigment or spread across the skin. It often looks like lighter or darker patches, and it can be itchy, scaly, or barely noticeable. Knowing how to spot it helps you.
The most common type is tinea versicolor. It’s caused by Malassezia yeast that lives on healthy skin but overgrows in warm, humid conditions. Patches usually appear on the chest, back, neck, or upper arms and may get more visible after sun exposure. Ringworm (tinea corporis) is another fungal cause that creates round, red rings with clearer skin in the center. Candida and other fungi can also cause color changes in skin folds and moist areas.
How do you tell fungal discoloration from other causes like eczema or vitiligo? Look for texture and pattern. Fungal patches often have fine scaling and a clear border, or tiny clustered spots. Vitiligo causes total loss of pigment with smooth edges and no scaling. Eczema is more inflamed and often very itchy. If the patch responds to antifungal shampoos or creams within a few weeks, that’s a good clue it’s fungal.
Over-the-counter options work well for many cases. Topical antifungals with clotrimazole, miconazole, or terbinafine are effective for tinea corporis and some skin yeast infections. For tinea versicolor, selenium sulfide lotion or ketoconazole shampoo used as a body wash two or three times a week can clear the fungus and help pigment return. Apply products to clean, dry skin and follow the label. Expect the fungus to clear before skin pigment fully recovers; pigmentation can take weeks to months to normalize.
If OTC treatments don’t help in two to four weeks, see a clinician. They may confirm the diagnosis with a skin scraping under a microscope or Wood’s lamp and prescribe oral antifungals like fluconazole or itraconazole for more stubborn or widespread infections. People with weakened immune systems, diabetes, or recurrent infections should get medical advice sooner.
Prevention is simple and practical. Keep skin dry in humid weather, wear breathable fabrics, change sweaty clothes quickly, and use antifungal body washes during hot seasons if you get recurrent flare-ups. Avoid sharing towels and clothing until the infection clears. For swimmers or gym-goers, dry off fully and put on fresh clothes.
When to see a doctor: if the patches spread rapidly, are painful, blistering, very itchy, or don’t improve with OTC treatment. Also seek care if you’re unsure about the diagnosis or if the discolored area affects your self-esteem — treatment options and counseling can help.
Fungal skin discoloration is common and usually treatable. With the right product and simple habits, most people see improvement. If you’re unsure which product to pick, a pharmacist or doctor can point you to the best option for your skin type and condition.
Protect the treated area from strong sun while pigment returns; use SPF 50+ and loose clothing. Follow up with your clinician if spots return after a few months for further advice.
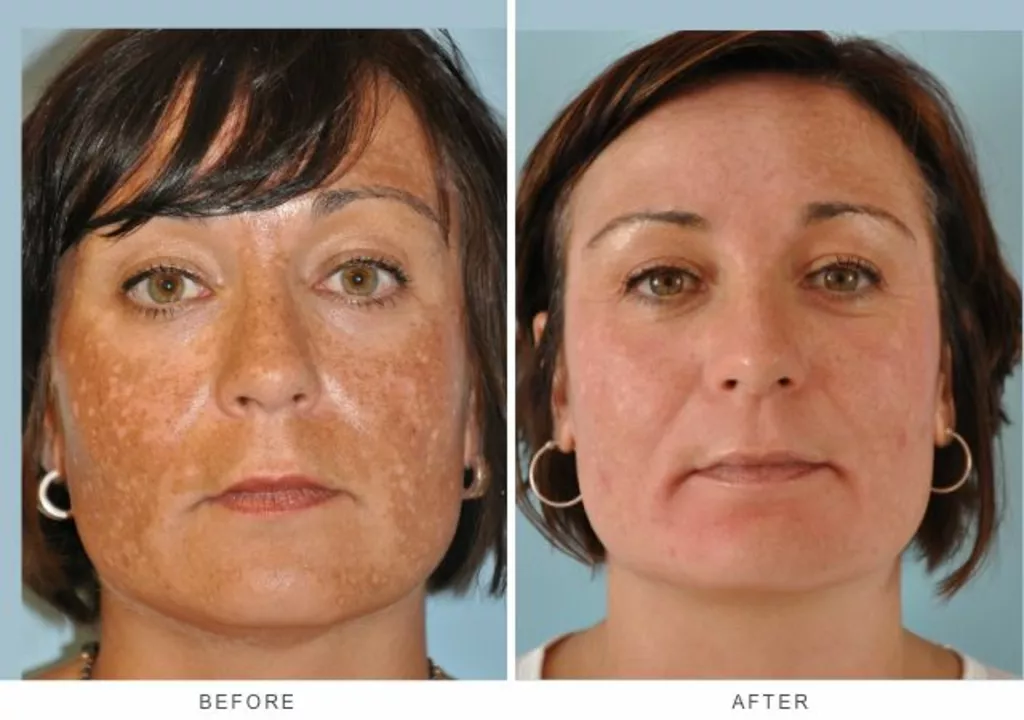
In my latest blog post, I discussed the significant role humidity plays in promoting fungal skin discoloration. I found that damp and humid environments create the perfect breeding ground for fungi, which can lead to skin issues like discoloration and infections. It's essential to maintain proper hygiene and keep our skin dry to prevent such problems. I also suggested some practical tips to reduce humidity at home, such as using a dehumidifier and ensuring proper ventilation. Overall, understanding the link between humidity and fungal skin discoloration can help us take better care of our skin and avoid unsightly and uncomfortable issues.
